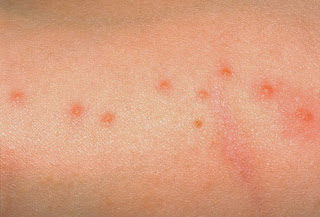
If you’re noticing red spots creeping up on your baby or child’s skin, do not panic.
Childhood rashes are a common occurrence in babies and young children as their skin is highly sensitive and easily affected by external factors such as dryness, bacteria, changes in the weather or contact with various allergens.
Some common skin conditions in babies and children are eczema (atopic dermatitis), diaper rash, hives (urticaria), contact dermatitis and heat rash.
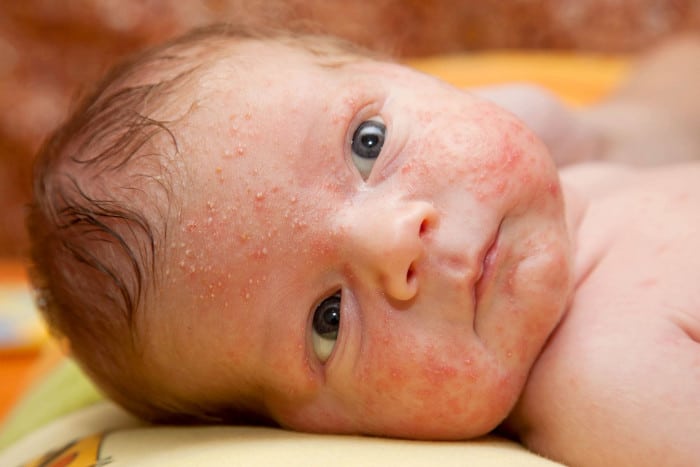
- Eczema
Eczema, or atopic dermatitis, is a dry, itchy skin condition that affects up to 1 in 5 children. It may surface in infants 3 months and above or during the childhood years. While most children will outgrow this condition, around 1 in 10 cases of eczema will persist into adulthood. This condition can also recur even after a dormant period.
Symptoms of Eczema
Eczema can appear as red, scaly and itchy rashes. In some instances, it may result in blisters with fluid and blood. Symptoms may also vary slightly depending on the child’s age.
In babies, eczema rashes usually present on the infant’s scalp and cheeks. In more severe cases, it can also spread to the limbs and torso. Babies with eczema may display distressed behaviour, such as rubbing their faces against the pillow or bed sheets in an attempt to soothe the discomfort.
In older children and adolescents, eczema commonly affects the flexural areas of the skin, such as the insides of the armpits, elbows, behind the knees, and groin area. However, it can also spread to more generalised areas in severely affected patients.
Contrary to popular belief, eczema is neither contagious nor a result of poor hygiene habits. Genetics are thought to play a role in causing allergic conditions such as eczema. Recurrent flare-ups may also be caused by triggers such as air pollutants, sweat, stress, food allergens or irritants coming into contact with the skin.
Managing Your Child’s Eczema
There are several remedies that can help relieve and prevent itching from eczema. Keeping your child’s skin moisturised daily with a fragrance-free moisturiser, ointment or lotion is an easy, common and effective treatment for eczema.
In addition, avoid strong soaps, chemicals and hot water while bathing as these can exacerbate dry skin conditions. Using a moisturising non-soap based body wash also helps to combat eczema. Your child’s doctor will be able to recommend suitable a range of moisturisers and body wash products that are suitable for eczema care.
If your child’s eczema is triggered by skin contact with irritants, avoid items and materials which can aggravate the itchiness. Keep your child’s fingernails short and tidy to prevent them from scratching.
Avoid wool and nylon clothing, and opt for cotton fabrics that are cooling, smoother and allow the skin to breathe. Avoid contact with objects like stuffed toys and carpets, and reduce dust mites around the house by keeping bed linen and curtains regularly washed.
Depending on your child’s age and condition, your child’s doctor may also prescribe topical steroids, oral anti-histamines or oral/topical antibiotics to reduce inflammation of the skin.
- Diaper Rash
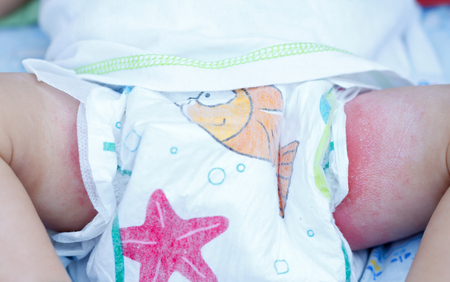
If the skin around your child’s diaper area appears red and irritated, your child is likely to have diaper rash, a common condition in babies around 9 to 12 months of age.
What causes diaper rash?
Diaper rash may develop as a result of moisture and bacteria from urine and faeces trapped in the diaper (irritant contact diaper dermatitis). This type of diaper rash appears red, shiny and on the buttocks instead of the folds of the skin.
Diaper rash can also be caused by a yeast infection (candida diaper dermatitis), which usually begins in the creases or folds of the thighs, then spreads outwards. It is usually red in appearance with satellite lesions.
Other common types of diaper rash include seborrhoeic diaper dermatitis and diaper rashes caused by impetigo, perianal streptococcal disease and allergic dermatitis. It is important to know that the symptoms of diaper rash may resemble other serious skin conditions. Hence, parents who are unsure are advised to see a doctor for a proper diagnosis.
Managing Your Child’s Diaper Rash
If your child has developed diaper rash, ensure their diapers are changed frequently or removed for a few days to allow the skin to air and heal. Clean your child’s diaper area properly by washing and patting dry during each diaper change. Limit the use of soaps and other harsh cleaners when washing your child’s diaper area.
Your child’s doctor may prescribe anti-fungal or antibiotics creams, anti-inflammatory creams or moisture-resistant ointment such as zinc oxide which forms a barrier over the skin to protect against stool and urine. Apply these topical treatments as instructed to help manage your child’s diaper rash.
- Hives
Hives, also known as urticaria, is a common skin condition in which red, itchy and swollen patches appear on the skin. These patches may be large or small.
What causes hives?
Hives appear when the body releases a chemical called histamine. Due to a variety of possible triggers, it may be difficult to pinpoint the exact cause of your child breaking out in hives.
Most cases of acute hives in babies and children are caused by a viral infection such as the common cold. However, hives may also be caused by an allergic reaction to foods such as peanuts, eggs, shellfish, soy, wheat or other nuts.
Other causes of hives include allergens such as pollen, animal fur, changes in temperature, or even medications such as non-steroidal anti-inflammatory drugs (NSAIDs).
Managing Your Child’s Hives
Hives may last for a few hours to a few days, with viral hives usually lasting for 1 to 2 weeks before gradually subsiding.
If your child’s hives have been caused by an allergen, strict avoidance of the food or medication is necessary upon advice from your child’s doctor. While most cases may not require medical attention, a doctor may prescribe oral antihistamines to alleviate the symptoms caused by hives.
If your child displays difficulty breathing, rapid facial swelling, is pale or cold to the touch, or is fainting or vomiting, this may be a sign of anaphylactic shock, a severe and potentially fatal allergic reaction. Seek immediate medical attention as emergency treatment may be needed.
- Contact Dermatitis
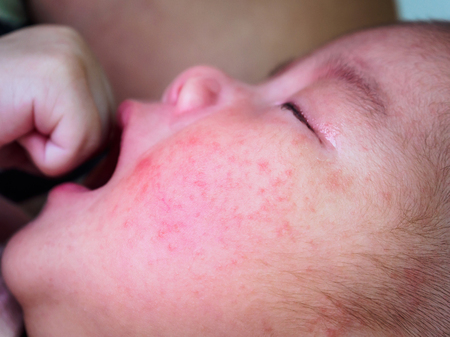
Contact dermatitis is a skin rash caused by contact with certain substances. These are either known as irritants, which cause a direct reaction or inflammation to the skin, or allergens, which trigger the body’s immune system to have an allergic reaction.
Some irritants which can trigger contact dermatitis in babies and children include urine and faeces in diapers (also known as Diaper Rash), saliva, soaps, baby lotions and detergents.
Allergens that cause contact dermatitis in babies and children include plants such as poison ivy or oak, metals such as nickel, chrome and mercury, latex which can commonly be found in rubber toys, balloons or pacifiers, and some types of medications.
Managing Your Child’s Contact Dermatitis
Rashes caused by contact dermatitis are usually most severe at the point of contact with the irritant (e.g. around the mouth and lips if caused by saliva)
Symptoms may vary according to individuals, but may typically include redness and skin swelling, blistering, itching or cracked, peeling skin.
Once identified, avoiding contact with the irritant is key to managing the occurrence of contact dermatitis. Wash skin thoroughly with soap after exposure and relieve inflammation with a cold compress on the skin surface.
- Heat Rash
Heat rash, also referred to as “prickly heat”, is an inflammation of the skin which occurs when the sweat glands are blocked and sweat produced is unable to escape.
This often takes place during hot and humid weather, if the child is overdressed or has increased temperature due to a fever.
A heat rash presents as small red bumps across the skin surface, like tiny blisters or pimples. It commonly occurs on the neck, diaper area, armpits, upper back and chest, where there are skin creases or lack of air circulation due to tight clothing.
Managing Your Child’s Heat Rash
A heat rash is not harmful and fades in a few days once the child’s skin has cooled down. This can be managed by removing excess clothing, using air conditioning, or placing a cool compress may be helpful.
Avoid applying lotion or creams on the skin as this may worsen the blockage of the sweat glands.
➡️ Related Read: My Baby Has Heat Rash
While these common skin conditions may seem serious and worrying to a new parent, the good news is, most of these conditions do not last till adulthood and will clear up on their own, sometimes with little or no treatment required.
However, in some cases, topical treatments such as moisturisers, creams, ointments or oral medications may be required to manage symptoms such as itch or inflammation of the skin.
This article is written by Dr Dave Ong, a paediatrician with special interests in allergies, skin conditions and respiratory problems in children. He practises at Kids Clinic (Punggol) and has weekend evening and Sunday appointments available.
* * * * *
Like what you see here? Get parenting tips and stories straight to your inbox! Join our mailing list here.
Want to be heard 👂 and seen 👀 by over 100,000 parents in Singapore? We can help! Leave your contact here and we’ll be in touch.