The skin is the largest organ in our body. It serves a critical function in preserving our bodily integrity. An infant or a child is not a miniature adult. At these extremes of age, the infant’s skin is constantly growing and maturing. On one hand, the skin’s immune system has yet to be fully developed, on the other, it is constantly being bombarded by harmful agents from the environment ranging from ultraviolet rays to bacteria and viruses.
What Are The Common Skin Problems In Newborn Babies?
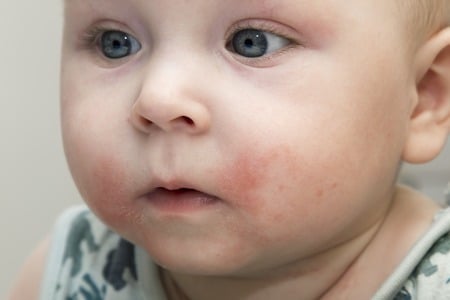
Eczema
Eczema is a dry, itchy skin condition that can affect up to a third of children in developed countries. There are many types of eczema and can be broadly classified into the internal type (endogenous) or the external type (exogenous) eczema. The majority of eczema affecting children is a type of endogenous eczema commonly known as atopic eczema or atopic dermatitis. It is closely related to conditions such as asthma and allergic rhinitis.
Atopic eczema is a skin condition with a very strong genetic influence. This means that if a parent or sibling has atopic eczema, the baby is at higher risk of developing atopic eczema. The majority of children with atopic eczema will present with dry and itchy skin by the age of one.
There may be episodes of flare-up where the rash becomes weepy, painful and is causing distress to the baby or child. Babies tend to get the rash over their cheeks, necks and elbows whereas older children tend to have their rash in front of their elbows or behind their necks.
Management of atopic eczema requires an individualised treatment plan. Often, the plan will include an anti-inflammatory cream, a moisturiser and anti-itch medications. In more severe cases, oral antibiotics and systemic treatments may be necessary. In cases where the control of eczema remains good, there is a good suggestion that eczema will clear up during the adolescent years.
⇒ Related Read: All-Natural Skincare to Protect Your Baby’s Delicate Skin
Milia
Milia are tiny, white spots that may appear on the baby’s face. Affected areas may include the nose, cheeks, chin, forehead, or around the eyes. They normally appear a couple of weeks after birth because the oil glands on the baby’s face are still developing. Milia spots should clear up on their own within a few weeks. Do not try to squeeze them or do “extraction” treatment.
Cradle cap dermatitis
Cradle cap dermatitis is a fairly common skin condition affecting newborns. The baby will have a red rash affecting the scalp and the rash can sometimes end up with very thick scales covering the scalp. These thick scales may flake off, in a way very similar to what we see in adult dandruff. Sometimes these scales may have some hair attached to them when they fall off. Not to worry, cradle cap does not cause baldness in babies.
Cradle cap dermatitis can occasionally affect other parts of the baby including the face, neck and groin areas. The thick flaky scales may improve with washing the hair regularly with a very gentle shampoo. In more severe cases, short-term use of a mild medicated shampoo may be required.
Baby acne
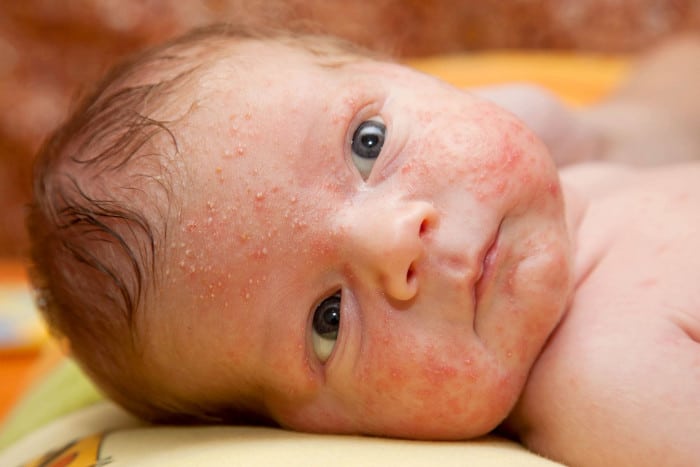
You will be surprised to learn that babies can get pimples too! Baby acne may be present at birth but usually appear a few weeks after birth. It looks like small pimples or whiteheads most commonly appear on the baby’s cheeks. These pimples may sometimes also affect the chest and back.
Baby acne comes about because of the baby’s exposure to the mother’s high level of female hormones during pregnancy. The high level of female hormones mimic a “puberty” in the baby and causes these pimples to form.
Baby acne will disappear on its own without any treatment although this may take weeks, sometimes even a few months. In severe cases, a topical cream may be helpful. As for the mother, there is little she can do to predict or prevent the development of baby acne. Neither the diet of the mother nor the baby will affect baby acne.
➡️ Related Read: Choosing Newborn Baby Skin Care Products
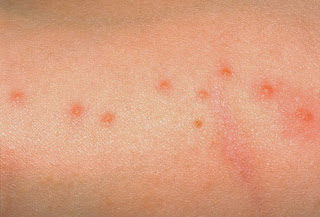
Nappy rash
Nappy rash is a form of eczema that affects the baby’s genitals, bottom, and folds of the thighs. It causes a red puffy rash which can sometimes look pimply. The rash can either by wet or dry. It is more common during the first year of life and persistent skin wetness is usually the main cause of nappy rash. Urine and diarrhoea are some of the common reasons for nappy rash. Sometimes, complications may occur where the rash becomes secondarily infected either by yeast or bacteria.
➡️ Related Read: Vomiting Or Diarrhoea In Children: What Food To Feed Your Child
Hence it is important to keep the area clean and dry by changing the diapers regularly. Treatment involves using anti-inflammatory creams. Where there is a suggestion of secondary infection, your doctor will prescribe the appropriate medication to clear the infection.
Molluscum contagiosum
Molluscum contagiosum is a viral infection of the skin. It can affect both infants and small children. The rash appears as small, round, shiny, pearly white or pinkish spots, some with a dimple in the middle. The spots are usually a few millimetres wide. New spots may develop over several weeks and they may cause itch in some cases. Common areas include the face and trunk. Sometimes the arms and legs can also be affected.
Molluscum contagiousum can clear up without treatment but this can take up to 18 months. The doctor can discuss some of the treatment options available which have to take into consideration the age of the child. Even with treatment, it typically takes a few weeks for the infection to clear up. Recurrence is not uncommon.
By Dr Gavin Ong, Medical Director and Consultant, The Skin Specialist (A subsidiary of Singapore Medical Group).
This article was first published in The New Age Parents e-magazine.
* * * * *
Like what you see here? Get parenting tips and stories straight to your inbox! Join our mailing list here.
Want to be heard 👂 and seen 👀 by over 100,000 parents in Singapore? We can help! Leave your contact here and we’ll be in touch.