Welcoming a newborn into the household is filled with much excitement, hard work but it also comes with a degree of uncertainty. What does the hard work entail? There are regular prenatal check-ups to schedule, tests and scans to undergo, prenatal classes to attend, nursery rooms to deck out and of course, preparation for the delivery of the baby.

Depending on the mother (and baby), some pregnancies are smooth-sailing, while others may face challenges and unpredictable deviations from their desires and plans.
Most women in their first pregnancy will be expecting a smooth prenatal course, followed up an uneventful normal vaginal delivery. However, some may be surprised when they learn of pregnancy-specific conditions that they encounter for the first time, such as gestational diabetes, pre-eclampsia, placentation problems, growth restriction of the baby, etc.
For common conditions like these, the prenatal follow up may have to be tweaked to suit the conditions, likewise, the delivery process may also differ from their expectations.
Caesarean sections are one of the most commonly performed surgeries that women undergo in their lifetime. It involves an abdominal incision to reach the womb, in order to deliver the baby in the most expedient manner. It may be performed electively or as an emergency recourse when vaginal delivery is hampered.
As the course of labour can change very suddenly, I routinely set aside some time during the regular prenatal visits to explain to my expectant mothers about the conduct of caesarean section, risks and benefits compared to vaginal delivery and possible scenarios that this option might have to be considered.
➡️ Related Read: C-Sect: A Life-Saver Or Just Another Birth Option?
Providing the necessary information will empower mothers to make their own decisions regarding the mode of delivery. In a local poll, although many women hope to have a vaginal delivery, a significant proportion (up to 60%) may end up requiring a caesarean section, commonly for reasons such as fetal distress and baby being too big to pass through the birth canal.

The vast majority of caesarean sections are performed either with spinal or epidural anaesthesia; general anaesthesia is rarely used, unless in specific emergency situations. As such, most mothers (and fathers) will be able to hear, touch and carry the newborn baby immediately after delivery, without fear of feeling any pain from the surgery site.
The preparation for a caesarean section starts with setting an IV drip and shaving the pubic hair (only for women with a high pubic hairline that encroaches into the incision zone, which is typically just below the level of the “bikini line”).
Oral medicine to neutralise the gastric acid is usually served before transiting to the operating theatre. Upon reaching the theatre, the anaesthetist will administer the spinal or epidural anaesthesia, before a urinary catheter is inserted. Once adequate anaesthesia is achieved, surgery will commence.
Following the skin incision, the surgeon will get through various layers of the abdominal wall and the womb to reach the baby. Thereafter, external pressure will be applied to the mother’s upper abdomen, to push the baby out from the caesarean incision. The umbilical cord will be clamped and cut when the pulsation has stopped, then the placenta will be removed from the womb.
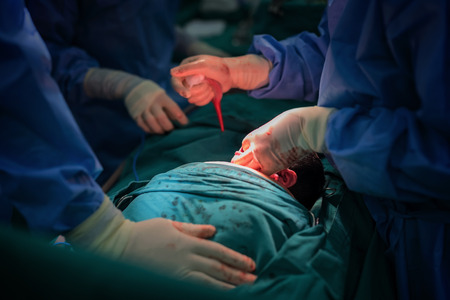
Closure of the womb and abdominal wall will be done in layers to restore the original anatomy. For most cases, an adhesion deterrent barrier will be applied to the surgery site to prevent scarring, where adjacent structures such as bladder and intestines “stick” to the healing womb, causing problems in future.
While the mother is having her caesarean wound closed up, the baby will be dried and wrapped in warm, clean towels by the attending midwife. Weight and other measurements of the baby will then be taken before the baby is handled to the parents, for the precious Kodak moment or even the initiation of skin-to-skin bonding and breastfeeding.
Closure of the caesarean skin incision is a very personal choice of surgeon. I prefer to use buried sutures (invisible and no need to be removed after surgery) in multiple layers to reduce tension. Wound tension is a major key factor to poor (ugly) wound healing. The final dressing will be a water-proof and anti-bacterial adhesion mesh dressing that will further minimise wound tension, for optimal healing.
This particular form of dressing is rapidly gaining popularity as it allows the patient to shower immediately after surgery without fear of wound disruption or infection. It is also very durable and does not need to be changed (maintenance-free). When removed 2-3 weeks after surgery, the underlying skin would have fully healed with very good cosmetic results too.
Other traditional methods of wound closure include non-absorbable sutures that require removal after a week or so, metal staples that also require the removal and leave the characteristic “centipede” scar, and glue or sticky tape (strips) for holding the wound edges together (with to without suture reinforcement)
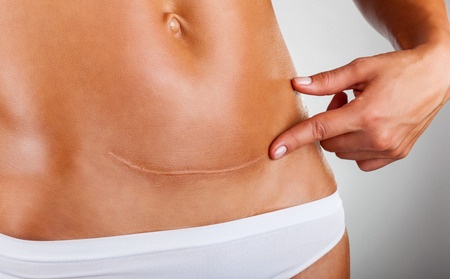
The typical caesarean section takes about 30-60 minutes from incision to birth and wound closure. Common post-operative side effects include abdominal cramps (womb contractions likened to menstrual cramps), nausea, uncontrollable shivering (not related to cold), weakness of the lower limbs (until the anaesthesia wears off fully) and fatigue.
It may be uncomfortable or hurt moderately when mommies cough, sneeze, or laugh, hence many will opt for a postpartum belt/binder for abdominal support and to reduce the discomfort of movement.
I routinely use these abdominal binders as an adjunct to reinforce the surgical wound closure, so that mommies can start to get active as soon as possible. Despite everything, caesarean section is still a major surgery and the tenderness should be expected to last for 2-3 weeks.
➡️ Related Read: Post-Partum Recovery: What To Expect
Although uncommon, new mothers who have just undergone caesarean section should be informed to watch for the following red flags during their recuperation: fever, severe pain over the surgery site, excessive vaginal bleeding and swollen legs that are painful to touch. These may herald serious complications such as infections and/or abnormal blood clots in the leg veins that require urgent attention.
Oral painkillers and sometimes antibiotics are served together with light meals a couple of hours after caesarean section when the patients are deemed ready for oral intake.
The usual advice given to patients is to begin exercising their lower limbs while still in bed after the surgery, this helps to improve blood circulation in the legs, hence reducing the risk for blood clots to form in the leg veins. Sometimes, a mechanical massager and/or injections to prevent blood clots are used, usually in high-risk patients.
➡️ Related Read: Professional Prenatal and Postnatal Massage at The Comfort of Your Home
Mothers are also strongly encouraged to start breastfeeding once they have settled down in their postnatal ward.

There is no need for them to pass urine, as a urinary catheter is usually in place to drain their urine into a bag. This prevents the bladder from overfilling before the anaesthesia wears off fully and the patient regains full sensation of their bladder.
The next 2 days are going to be packed with activities. The new parents will be introduced to their newborn, as well as a crash course on how to take care of them at home.
Parentcraft such as feeding the baby, bathing, changing diapers and swaddling will have to be picked up quickly, whilst the mother herself has to adjust quickly to the changes in her body after delivery. Having a reliable and maintenance-free wound dressing that allows her to be free to concentrate on the newborn is certainly bliss.
I often send my caesarean section patients home when the baby is 2-3 days old. The babies are usually discharged on the same day too, provided they are well and do not have jaundice that requires treatment.
This means the caesarean section only prolongs the hospital stay by 1-2 days, compared with vaginal delivery. There is no need for any change of dressing, tedious waterproofing of the dressing before shower or even abstaining from showering.
The end of the pregnancy journey should begin with the joys of parenthood, not the woes of wound care.
This article is contributed by Dr Steven Teo.
Dr Steven Teo is a gynaecologist and obstetrician with STO+G Practice at Thomson Medical Centre. He attained the specialist degree of Master of Medicine (O&G) from Singapore and became a Member of the Royal College of Obstetrics and Gynaecology (United Kingdom). As a specialist in KK Women’s and Children’s Hospital, Dr Teo had previously received various awards for exemplary performance in public service.
* * * * *
If you find this article useful, do click Like and Share at the bottom of the post, thank you.
Want to be heard and seen by over 100,000 parents in Singapore? We can help! Leave your contact here and we’ll be in touch.





















































