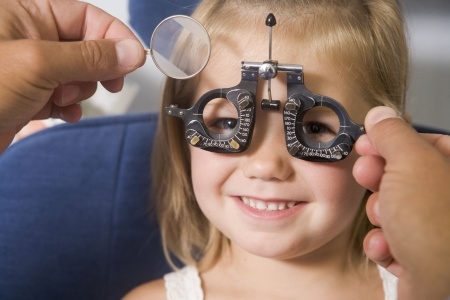
Having a happy healthy child is at the heart of every parent, and having a good vision is obviously one of the most important concerns.
Lazy eye, or amblyopia as it is medically referred to, is a common childhood condition to which occurs when the vision in one eye does not develop normally. It can occur in children between the ages of 2 to 3 and if not detected, can persist to cause one eye visual impairment which may occur at a later stage in the child’s growing and adult life.
The good news is that it is a reversible condition, and the key to this is early detection and treatment.
What Is Lazy Eye?

Proper vision requires both the eyes and the brain to be in good working order, as the brain processes the image signals conveyed by the optic nerves. Lazy eye occurs when the vision of one eye is reduced because the brain doesn’t seem to have such a strong connection with it as it does with the other eye.
What Causes Lazy Eye?
While any condition that prevents the eye from seeing clearly has the potential to cause lazy eye, one of the most common causes is the misalignment of the eyes or strabismus. This happens when the muscle behind the eye – which controls how they turn and move – becomes imbalanced. This causes both eyes to move in different directions, resulting in a condition commonly described as “cross-eyed”. Occasionally, lazy eye can also be caused by the clouding of the natural lens of the eye known as a cataract.
Lazy eye is also commonly associated with early-onset vision problems (refractive errors) such as near-sightedness (myopia), severe far-sightedness (hyperopia) and astigmatism. When the child has blurred vision at an early age and it is not corrected with prescription glasses, the unclear images sent to the brain are eventually suppressed, resulting in a lazy eye.
The role parents play in managing this condition is very important, and vigilance is needed to recognise the problem to get treatment for it as soon as possible.
Signs You Should Look Out For
While children seldom voluntarily complain of poor vision, there are signs parents can observe to help detect lazy eyes. Ask yourself:
- Does one of my child’s eyes stray away from the straight-ahead position when he or she focuses on an object?
- Do my child’s eyes seem to be working together or separately?
- Do my child’s eyes often cross?
- Is the child squinting a lot?
- How well does my child perceive the distance of an object? Hold an object at a distance and ask your child to reach out for it. If he or she is not able to judge the distance well, it may be a sign that both eyes are not working well together.
What Can Be Done To Treat Lazy Eye
Lazy eye treatment can vary depending on the cause of the problem and its severity. The treatment of lazy eye starts with treating all the underlying issues preventing the eye from seeing well (i.e. cataracts, strabismus and refractive errors) and compelling the affected eye to send clear images to the brain.
Patching

A patch is worn over the better-seeing eye for weeks to months. This therapy forces the child to use the eye with lazy eye. Patching stimulates vision in the weaker eye and helps parts of the brain involved in vision to develop more completely. The child only has to wear the patch a few hours a day, which can be done in the privacy of the home.
Atropine
A drop of a drug called atropine is placed in the stronger eye to temporarily blur vision to make the lazy eye work harder, particularly when focusing on near objects. This is obviously less conspicuous and can be just as effective, making it sometimes easier for parents and children to use, though some children may experience some eye irritations.
Early intervention is key to treating lazy eyes in children, particularly because if left untreated it often persists into adulthood with diminishing response to treatment. It is important for parents to be aware of the symptoms of lazy eye, as early detection would give the child the best possible chance of vision recovery, which is crucial for the future of your child’s eyesight.
Encouragement and support in the treatment process are also very important, so that child feels comfortable and happy to know that this is just part of the process of helping them see better.
This article is contributed by Dr David Chan, Senior Consultant Ophthalmologist and Medical Director of Atlas Eye Specialist Centre.
* * * * *
If you find this article useful, do click Like and Share at the bottom of the post, thank you.
Like what you see here? Get parenting tips and stories straight to your inbox! Join our mailing list here.