Arthritis is not a condition reserved for the elderly.
Cases of Juvenile Arthritis have been growing and today there are about 500 cases reported. An autoimmune disorder, these children experience swelling, pain and stiffness in the joints.
Yet, due to the lack of familiarity with the disease, many parents and healthcare professionals are unable to identify, diagnose and treat the condition.
We asked an expert to find out more about how this health condition can affect children.
What is Juvenile Arthritis?

It is a chronic condition causing inflammation in any joint in the body, starting before the age of 16 years old.
When left untreated, the inflammation can cause joint damage.
We don’t know the exact cause of arthritis, which is what the term “idiopathic” in Juvenile Idiopathic Arthritis (JIA) means. Scientists are still looking for the causes of juvenile arthritis.
It is most likely an autoimmune disease. This means that the body’s immune system, which is meant to fight off infections, starts to attack its own healthy cells and tissues.
The immune system is meant to defend itself by causing inflammation and swelling. In juvenile arthritis, the body creates inflammation in joint(s) where it doesn’t need to. This means that the white blood cells produce chemicals that harm the lining of the joint.
There is no proof that diet, allergies, stress, vitamin deficiencies are the cause of Juvenile Idiopathic Arthritis, JIA. There is a genetic predisposition to JIA, but genetic markers alone cannot predict who will get arthritis.
Scientists believe that a trigger, like a virus, can set off the disease process in children with the genetic tendency.
What are the symptoms?
The most common symptoms of juvenile arthritis are joint swelling, pain, and stiffness of the joint. Any joint may be affected, but the knees, hands, feet are most commonly affected. The symptoms are usually worse in the morning, after prolonged sitting or a nap.
Not all children with juvenile arthritis will have the same symptoms. Some symptoms are specific to a subtype of JIA. Symptoms may change from day to day, or even within the same day. Children will have times when the symptoms go away (remission) or get worse (flare).
Other signs may include:
- Limping in the morning
- Clumsiness, reduced physical activity
- High fever and skin rash
- Swelling in the lymph nodes and other parts of the body
- Sometimes, the affect joint may feel warm
Can it be prevented?
Unfortunately, it cannot be prevented.
Who gets affected?
There are about 500 children with JIA in Singapore and the typical age range is 2 to 16 years old. The youngest patients are infants, but this is rare.
NUH sees about 70 – 80 active patients in total. The number of children going to Paediatric Rheumatology Clinics for evaluation of joint pain is about twice as many as those with JIA.
JIA is the most common form of chronic arthritis in kids. It occurs in children aged 16 and below and has seven subtypes. The earliest onset witnessed was 4 months.
Depending on the subtype, the gender predominance differs; e.g. in ERA, boys are more commonly affected. In rheumatoid factor positive poly JIA, girls are more affected. In systemic JIA, the sex ratio is equal. This is because JIA is a really heterogeneous disease, even if they are lumped under one big umbrella term of “JIA”.
How is it diagnosed?
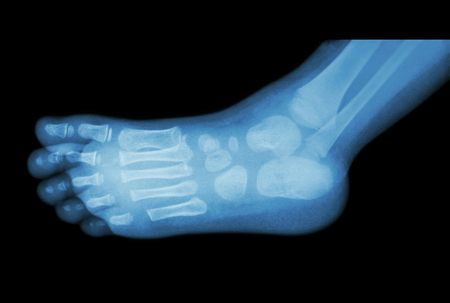
Arthritis is diagnosed based on history (what the patient tells doctors) and a physical examination. X-rays may indicate the severity of the disease. An ultrasound or magnetic resonance imaging scan may help to confirm the diagnosis.
Blood tests are not useful for diagnosing arthritis and the result may only be abnormal if there is widespread joint involvement. They are done only when a child is diagnosed with arthritis to get clues to the prognosis.
What are the treatments?
Non-steroidal anti-inflammatory drugs like ibuprofen naproxen are used in arthritis for their anti-inflammatory effect, and the reduction of pain is one indication that the inflammation is subsiding.
Many new drugs have been developed in the past 15 years which allow children to get good control of their arthritis with fewer side effects. These drugs, known as biologics, must be given as injections or infusions.
New biologics have been approved in the last 5 to 10 years, including a class of medicines that can be given orally. Some of the newer biologics are given less frequently, which means fewer injections for the children.
Thanks to biologics, doctors can now control close to 100% of JIA. When JIA is treated early, complete remission, often with medication, is possible. However, delays in achieving remission prolong the period of symptoms, which mean more days of pain, reduced physical activity, missed school, etc.
Reasons for delays are many; difficulty from parents in accepting need for long-term medication, family resistance to high cost of biologic medicines. This is why the CapitaLand-NAF Juvenile Arthritis Fund was set up, to assist needy families defray the costs of the expensive biologic medicines.
How can parents or families help a child live comfortably with Juvenile Arthritis?
Early treatment and remission can get the child the best outcome, and ensure healthy joints into adulthood. Feel free to ask your doctor questions and discuss your thoughts.
Besides being involved and supportive of the doctor visits and treatment, encourage your child to be active when the joints are in remission, have a healthy diet and lifestyle together as a family, stay positive.
Patients are advised to maintain a healthy, balanced diet for overall good health and to prevent obesity. Being overweight will put additional stress on the joints. Once the arthritis is under control, the child should be allowed to do all the physical activities and sports he wants.
In fact, regular physical activity will help to reduce the pain of arthritis and allow the child to develop strong bones and muscles.
These questions were answered by Dr Elizabeth Ang. Dr Ang is a Paediatric Consultant in the Division of Allergy, Immunology and Rheumatology, Paediatrics, National University Hospital and Assistant Professor in the Department of Pediatrics, National University of Singapore.
* * * * *
Like what you see here? Get parenting tips and stories straight to your inbox! Join our mailing list here.
Want to be heard 👂 and seen 👀 by over 100,000 parents in Singapore? We can help! Leave your contact here and we’ll be in touch.