Jaundice is the yellowish discolouration of the skin, most obviously seen in the whites of the eye, caused by elevated bilirubin levels in the blood. Bilirubin in the blood is normally removed by the liver and it leaves the body through urine and stool. About 50 to 80 percent of newborn babies develop jaundice in the first week of life, as their liver takes a few days to mature before bilirubin can be removed efficiently. Most babies have mild jaundice, it resolves spontaneously without causing major problems.
However, jaundice in babies should be taken seriously, as very high levels of bilirubin can cause brain damage leading to long-term problems. All babies with jaundice should be monitored by a doctor or nurse.
Causes
Jaundice occurs in newborn babies as there is more bilirubin in the blood than they can get rid of.
The commonest cause of jaundice in newborn babies is physiological jaundice (there is no underlying disease). This is the result of increase bilirubin from breaking down of blood cells, in combination with immature liver to remove the bilirubin. This cause of jaundice normally appears within 2 to 4 days of birth, tends to disappear within 1 to 2 weeks in a full term healthy baby.
Breastfed babies are more likely to get jaundice than formula-fed babies, but this occurs mainly in babies who are not nursing well. Breastmilk jaundice can occur within 4 to 7 days of life in 1 in 10 breastfed babies, persisting longer than physiological jaundice. This should be distinguished from breastfeeding jaundice, which tends to occur in first 3 days of life as a result of dehydration from inadequate intake of breastmilk.
Other possible causes are haemolysis (excess breakdown of red blood cells due to blood type incompatibility, G6PD deficiency), infection, bruising and metabolic or endocrine disorders (e.g. congenital hypothyroidism). Biliary atresia and congenital hyperbilirubinaemia syndromes (e.g Gilbert’s Syndrome, Crigler Najjar Syndrome) are rarer causes of jaundice in babies.
Symptoms
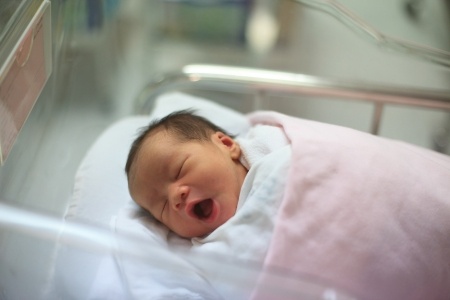
Jaundice is evident by the yellow pigmentation seen on the baby’s skin, whites of the eye and inner mouth. In darker skin babies, the yellow pigmentation on the skin may be difficult to see, except by looking at your baby’s eyes or inner mouth.
Lethargy, increasing sleepiness, difficulty arousing for feeding, a very high-pitched cry, poor suck, abnormal muscle tone or movements, fever, hearing loss, visual impairment can indicate dangerously high bilirubin level in the baby’s blood. If not treated promptly can lead to permanent brain damage and even death.
Pale stool and dark urine in jaundice babies may need further evaluation from your baby’s doctor as it can be due to more serious causes of jaundice.
Diagnosis
Your baby’s doctor will make a diagnosis and determine the cause of jaundice by first asking you about your baby and the mother’s health; and performing a physical examination of your baby.
If your baby has mild to moderate jaundice typically presenting on the second or third day of life, without any symptoms or signs suggestive of serious diseases; usually a blood test to determine the bilirubin levels is adequate. The blood test for bilirubin may need to be repeated, the repeat frequency will depend on the bilirubin levels, its trend and physical examination by your baby’s doctor. More tests might be required if your baby’s doctor thinks that there could be a health problem leading to high bilirubin in the blood.
Treatment

High bilirubin levels that exceed the normal range for your baby will be treated with phototherapy (light therapy). This involves exposing your baby’s skin under a blue light to break down bilirubin. This can be done in the hospital or at home. If your baby’s bilirubin reaches a critically high level, a procedure called exchange transfusion may be required. This involves taking out the blood slowly, replacing it with fresh blood without jaundice.
It is important to encourage adequate feeding and hydration of your jaundice baby, as this promotes elimination of the yellow pigments from the urine and stools. You will know if your baby has enough breastmilk or formula if he or she has at least 6 wet diapers a day, and the change of stool colour from dark green to yellow. You are recommended to continue and increase the frequency of breastfeeding, at least 8 to 12 feedings in the 24 hour period. If formula feeding, at least 6 to 10 feedings in 24 hours.
Breastfed babies who are dehydrated, continuing to lose weight excessively should have milk supplement with either more expressed breastmilk or formula. It is not recommended to put your baby under direct sunlight as there is a risk of overheating and further dehydration, as sunlight is not effective in reducing jaundice.
If your baby’s jaundice is caused by an underlying health problem like an infection, it needs to be treated. Occasionally, early surgery may be indicated if the baby’s jaundice is due to more serious problems like biliary atresia.
Dr Yong Lok Sze is a General Practitioner of Lifescan Medical (formerly known as SMG Medical), a subsidiary of Singapore Medical Group (SMG). Her proactive approach to acquire updated advances in medicine and upgrading her skills as a physician has benefited her patients in many ways. Providing the best medical care to her patient is Dr Yong’s main consideration.
* * * * *
Like what you see here? Get parenting tips and stories straight to your inbox! Join our mailing list here.
Want to be heard 👂 and seen 👀 by over 100,000 parents in Singapore? We can help! Leave your contact here and we’ll be in touch.























































